Oral cancer
Oral cancer is on the rise
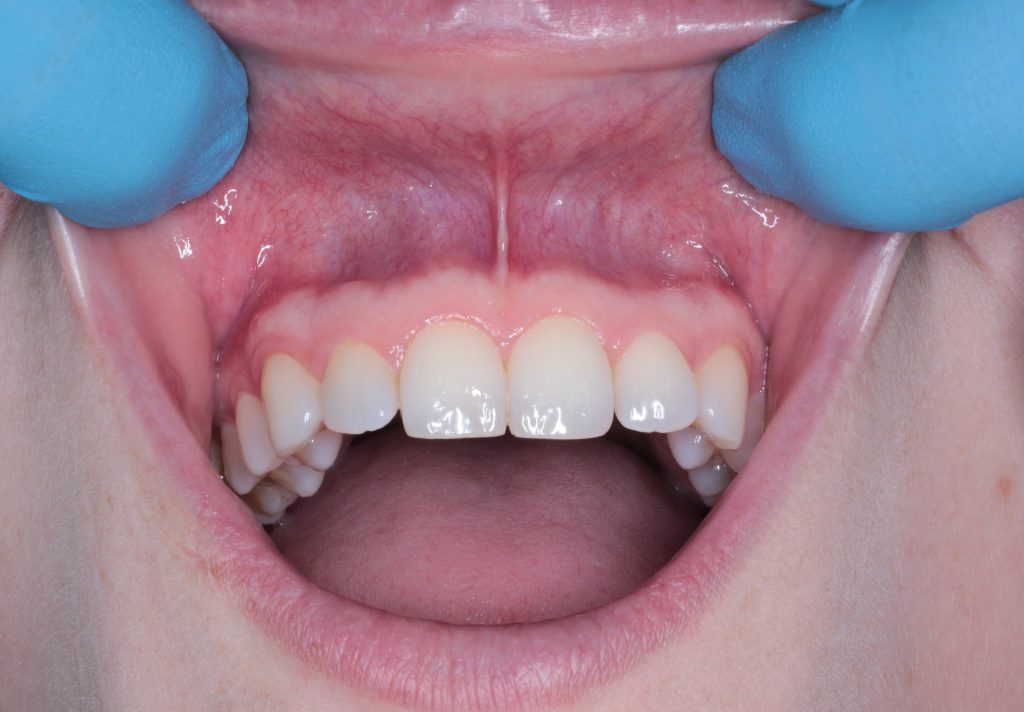
The incidence of oral cancer in the UK has risen by 97% over the last 20 years to over 8,700 cases each year, and numbers are expected to continue increasing.
The vast majority of cases are linked to lifestyle factors, mainly use of tobacco or alcohol, but also an unhealthy diet, exposure to ultraviolet light, and behaviour resulting in infection with human papillomavirus (HPV).
Public awareness of oral cancer is relatively low, and diagnosis is often late, with almost half of oral cancers diagnosed only once the cancer has already spread to another part of the body.
The number of people dying from oral cancer has risen by almost half over the last ten years to over 2,700 per annum.
Dental teams have a vital role
However, if the disease is detected and treated early, survival rates over five years can almost double, and dental professionals can play an important role in early detection and referral. Dental professionals also have an important role in maintaining the oral health of patients who have undergone treatment, sometimes radical, for oral cancer:
- Dental teams should ensure they know the signs and symptoms of oral cancer, and should familiarise themselves with relevant national guidelines and resources
- The face, head and neck should be examined, as well as intra-oral soft tissues, during a routine examination. Clinicians should be vigilant about cancer of the head and neck as well as oral cancer
- Practices should ensure they are familiar with their local referral pathways for suspected oral / head and neck cancers, that all staff are aware of how to refer, and should be ready to give patients written information to take away to encourage them to attend their referral appointment
- Practices also have a vital role in raising awareness among their patients of the risk factors for oral cancer, and of how to carry out a regular self-check
- Practices can encourage patients to adopt less risky lifestyles, in particular to stop smoking and keep alcohol consumption within recommended levels
Guidelines and resources
Clinical Examination and Record-Keeping: Good Practice Guidelines, published by the College of General Dentistry, recommends that clinicians examining patients should look for signs of oral cancer, as well as examine the face, head and neck, as part of the routine oral examination, and make a referral where they suspect a patient may have cancer or a pre-cancerous lesion. This is freely available to all dental professionals.
Section 4.3 details how an extra-oral examination should be carried out and recorded, and section 4.4.1 details how a soft tissue examination should be carried out and recorded. Section 7.1.2 covers urgent referral, and Section 3.4 defines the socio-behaviour history that should be recorded on the medical history form, including tobacco and alcohol use. Appendix 8A is a soft tissue examination checklist; appendix 8B is an example of a soft tissue lesion monitoring chart; and appendix 8C is an example of a soft tissue examination mouth map and chart.
Chapter 6 of Delivering Better Oral Health: an evidence based toolkit for prevention, published by the Office for Health Improvement & Disparities (formerly Public Health England), covers the epidemiology of oral cancer, summarises the strength of the available evidence on risk factors, and advises dental teams:
- to ‘ask and examine’ all patients
- of the signs and symptoms of oral potentially malignant disorders
- how to make referrals for a suspicious mucosal lesion or potential oral malignancy
- how to ‘advise and act’ in relation to high risk patients
- of the need for dental care before and after treatment for cancer
In the recently published fourth edition, Chapter 2 includes a new summary table on prevention of oral cancer. Chapter 3 covers behaviour change, Chapter 11 smoking and tobacco use, and Chapter 12 alcohol consumption.
Statement 4 of Quality Standard 124, published by the National Institute for Health and Care Excellence, recommends that ‘people with suspected cancer who are referred to a cancer service are given written information encouraging them to attend’.
The Oral Cancer Recognition Toolkit, developed by Cancer Research UK and the British Dental Association, includes a referral decision guide and lesion recognition resource. This is freely available to all dental professionals and comes with CPD hours.
The Royal College of Surgeons of England and British Society for Disability and Oral Health publish guidelines on The Oral Management of Oncology Patients Requiring Radiotherapy, Chemotherapy and/or Bone Marrow Transplantation.
Mouth Cancer Action Month, organised by the Oral Health Foundation, is a campaign every November to raise public awareness of oral cancer, highlight the risk factors, educate people on what to look for and how to perform regular self-checks, and encourage those who see anything unusual to visit their dental practice as soon as possible. Downloadable posters highlighting these messages, and images for use on social media, are made available free of charge, and we would also encourage dental professionals to buy and wear the charity’s Blue Ribbon badges in order to support its important work, and to help raise awareness of oral cancer among your patients, colleagues, friends and family.
ProDental CPD has produced a number of relevant webinars to which College members have free access on-demand:
- Early Detection of Oral Cancer
- Mouth Cancer – Diagnosis and Breaking the News
- Mouth Cancer – Treatment and Ongoing Care
- Basic Oral Care for the Mouth Cancer Patient
- Prosthetic Rehabilitation of the Head and Neck Cancer Patient
- Stopping Smoking – Guide for the Dental Team
Health Education England’s Alcohol (Identification and Brief Advice) for Dental Teams module aims to help dental professionals to engage effectively with patients who drink above recommended levels, but who are non-dependent and may not realise that their drinking might impact their health. The training has been designed to enable this to be undertaken in only take a few minutes by using a three-question screening test and delivering routine, structured advice aimed at reducing consumption. Those not already registered to use the NHS’s e-Learning for Health portal will need to create an account and validate their email address, and once logged in should click ‘My Account’, then ‘Enrolment’, select the module and then access it from ‘My e-Learning’. NHS staff in England and Wales can access it via their Electronic Staff Record.
For further information, see:
The State of Mouth Cancer UK Report 2020/21: https://www.dentalhealth.org/Handlers/Download.ashx?IDMF=33f0d4c5-aa47-4e06-9454-9914e2476614
Mouth Cancer Foundation website: https://www.mouthcancerfoundation.org/
Oral Health Foundation mouth cancer pages: https://www.dentalhealth.org/mouthcancer
British Dental Association oral cancer information and resource page: https://bda.org/oralcancer
Image courtesy of Vita Tanden
Join us | Sign up for College newsletter | Member register | Register of supporters
Privacy policy | Cookie policy | Patients and public | Contact
College of General Dentistry (CGDent), Kemp House, 152-160 City Road, London, EC1V 2NX
Company Registration No. 2586636 | Registered Charity No. 1002769

