In collaboration with his practice Principal, Francisco Casserley, Choudhury Rahman (BDS, Manchester 2023) discusses why informed patient consent and accurate record‑keeping are essential, and shares his practical advice on the key points early career clinicians should consider.


Something which worries many new dentists is the issue of litigation. We all dread that moment we get an email or a letter about a patient who is unhappy with something which we have done, or is wishing to make a complaint. One of the ways we can help ourselves is by ensuring we have really good consent, and clear record-keeping. Both of these things go hand-in-hand, and in this blog I will discuss how we can ensure we are protecting ourselves well.
Disclaimer: This is not an exhaustive guide to consent or record keeping. These are my suggestions based on my personal experience as a young dentist. I would recommend referring to the CGDent guidance on Clinical Examination and Record-Keeping, or undertaking CPD to ensure you gain a good understanding of best practice in consent and record-keeping.
GDC principles and putting patients first
As undergraduates we will have spent a lot of time learning and understanding the GDC Principles. Many of these link together, especially back to principle 1 which is to “Put patients’ interests first”. This should be at the centre of everything we do and ties strongly into principle 3, “Obtain valid consent”.
What informed consent really means
Consent is not just asking the patient what they want to do, but it’s giving them all the possible options for treatment so that they are able to make an informed decision. Some of these options may be things you can’t undertake, for example, a tricky root canal treatment (RCT), a difficult extraction, crown lengthening to improve restorability, or even implants. The possibility of alternative options out of your scope, including private options, should be given to every patient. You shouldn’t let any pre-conceptions about the patient stop you from giving those options. Whether the patient goes ahead with any of those, is up to them, but you need to document clearly all the options you have given, along with what the patient has decided to do.
I’ve also seen many colleagues worry over giving the patient a recommendation of treatment. However, in Principle 3.1.3, the GDC says that it is fine to give your patient “your recommended option”. As long as the recommendation is clinically reasonable, it will always be appropriate to give them a recommendation based on your opinion and clinical scenario. Many patients also value your expertise and experience and will be happy to go with your advice.
Discussing risks, benefits and alternatives
It’s very important to discuss all risks and benefits with patients for each option of treatment so the decision they make can be informed. You need to have this discussion recorded in your notes with all the risks and benefits given. For example, if you have a particularly tough extraction for an upper molar which is close to the sinus, you need to advise the patient there is a risk of pain, bleeding, bruising and swelling. You would also need to advise there is a risk of tooth fracture, oroantral communication (OAC), damage to adjacent teeth and tuberosity fracture (if it’s an 8). I would also warn your patient that if a fracture occurs, they may need to be referred to see someone else to have any remaining bits of tooth taken out. If there was a particularly high risk of OAC, you may want to offer the patient the option to be referred for an extraction, so that if an OAC occurs, it can be repaired straight away. The reason to refer due to the higher OAC risk needs to be specified. The patient may be in pain, for example, and happy to accept this increased risk, but you need to make that option clear to the patient. This issue was highlighted in an article by the Dental Defence Union (the DDU).
Montgomery 2015 and material risk
Continuing on with specific risks to your patient, you need to have a good understanding of Montgomery 2015 and informed consent. This relates to the matter of “whether the information given to a patient is adequate, is judged from the perspective of a reasonable person in the patient’s position” and that “patients are aware of ‘material risks’” (MDU, 2024). I would recommend reading into the case and the issues that were raised, but to explain this simply for us as dental professionals, if there is an issue specific to the patient, and there is a risk with a procedure which can have particular consequences to them, it needs to be explained clearly to them.
For example, if you had a patient who was a chef, and taste is very important in their job, you may wish to warn them of the risk of lingual nerve injury from an inferior alveolar block. You should warn that this risk may result in temporary or permanent changes in their taste. With this risk in mind, you and the patient may decide on alternative ways to achieve analgesia for a dental procedure. This is only one example of the thought process you need to have when consenting a patient to treatment.
The importance of contemporaneous clinical notes
We all hate spending much of our time writing clinical notes, but there are many small details I have seen people miss. As mentioned in GDC Principle 4.1, “you must make and keep contemporaneous, complete and accurate patient records”. You need to ensure whoever is present in the room is recorded. This is particularly important in relation to paediatric patients in case safeguarding issues are being investigated. Any presenting complaints (PC) must be documented, along with the history of presenting complaint (HPC). These must be recorded in the patient’s own words. For example, if the patient says “I feel like ripping my tooth out”, put that in your notes in quotations. This could be important as it gives an idea of the kind of pain a patient might be in.
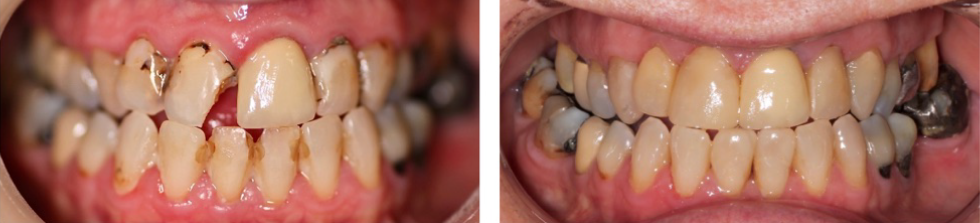
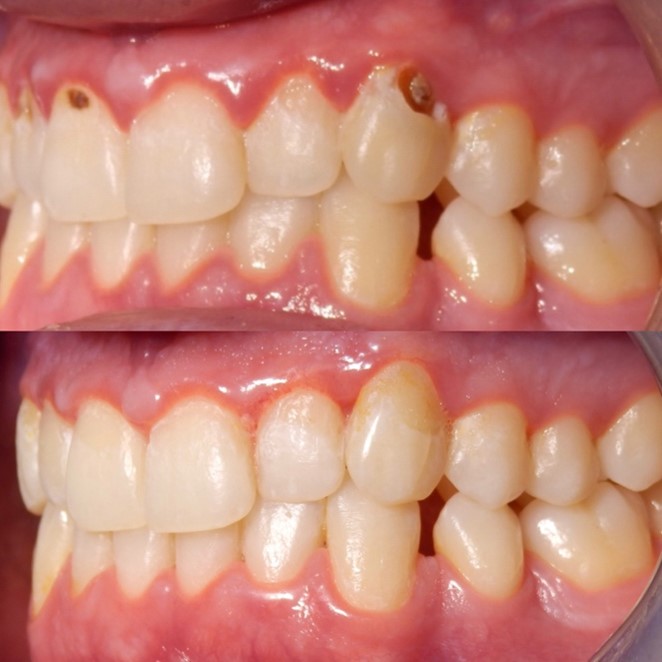
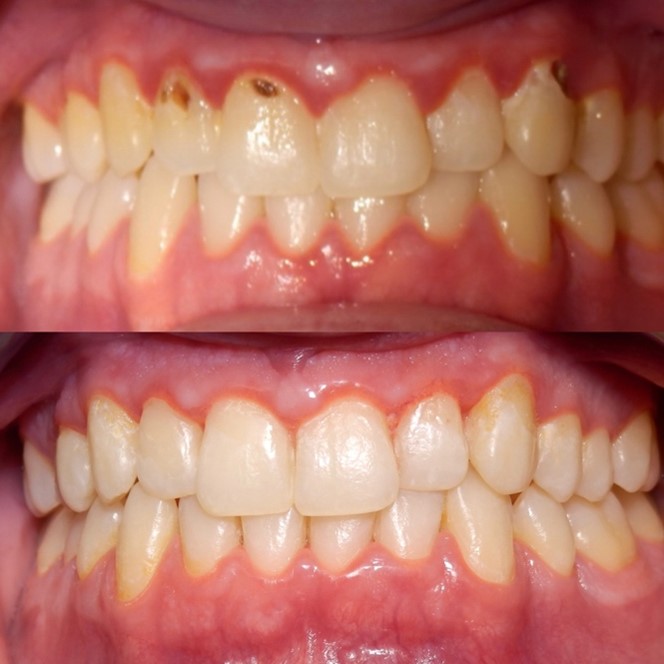
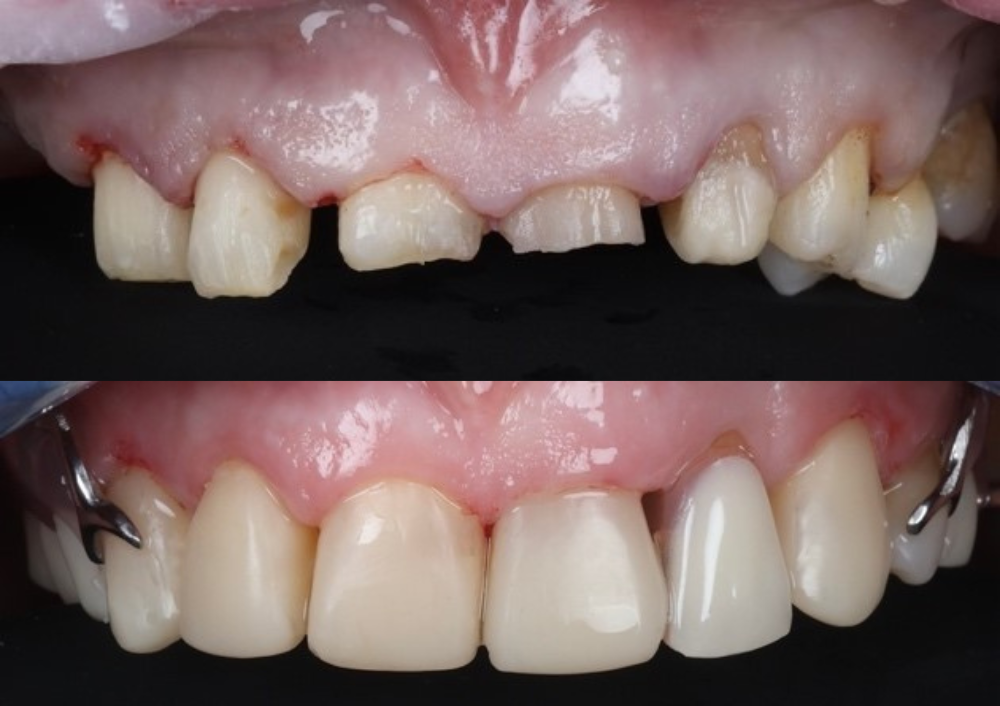
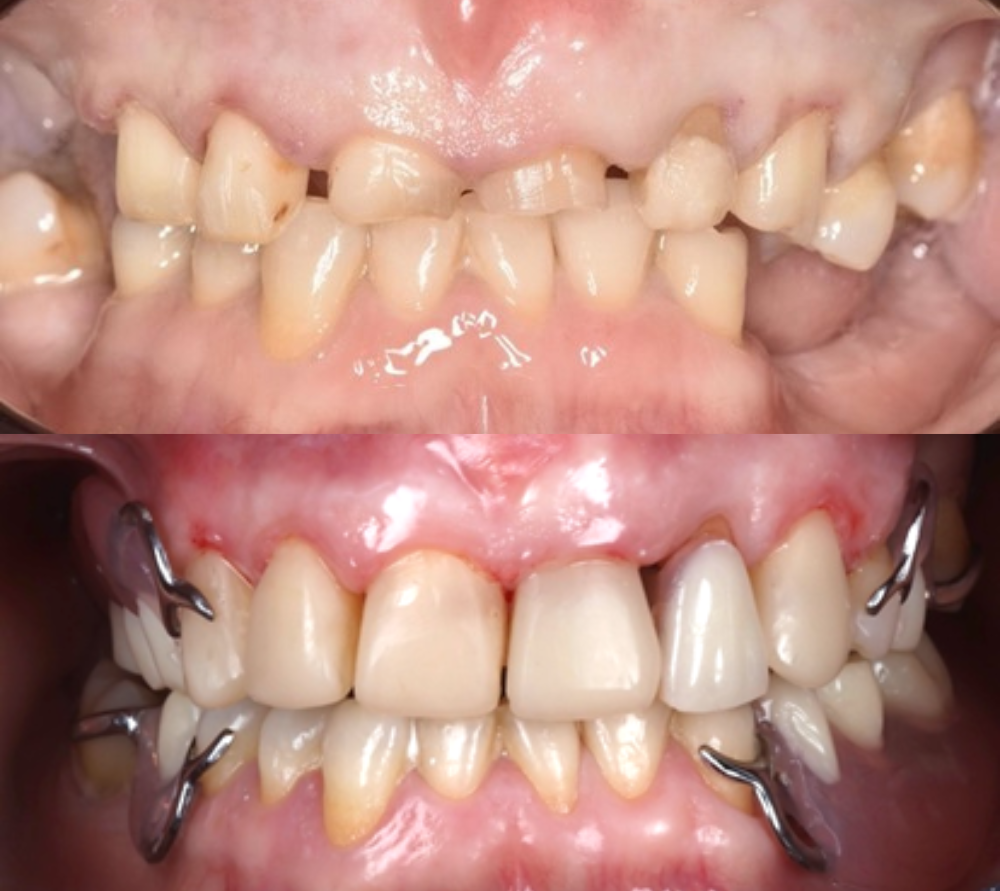
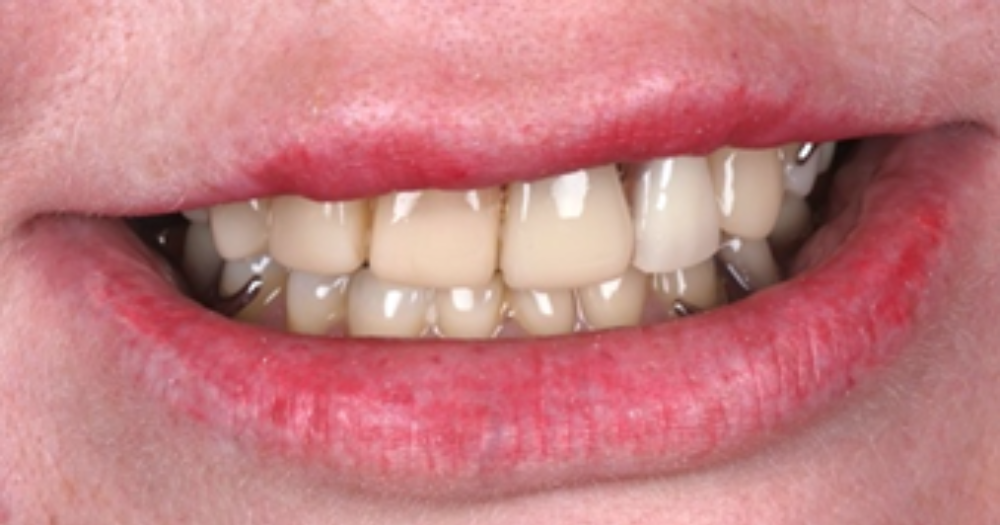
You should ensure you have clear notes of the patient’s medical history, social history (smoking and alcohol), dental history along with oral hygiene routine, findings in your exam/assessment, intra and extra oral findings, a comment on the oral hygiene, any special investigations taken with their findings including BPE, sensibility/TTP, Radiographs etc, risks level for caries, periodontal disease, oral cancer and tooth wear. You also need to record all your diagnoses (especially for periodontal disease with staging, grading and risk factors) along with treatment options and discussions. It is also great if you can take pre- and post-op photos of your work, or problems the patient is attending with, as this can show how the patient has presented to you – this a form of evidence which is indisputable if there are issues afterwards or concerns about the care you have provided. Top tip – make sure your camera’s date and time settings are correct before taking the photos. Find out about how to pick a good camera set up in my blog ‘How to get the most out of Foundation Training and make the right investments’
Templates can be a great tool, especially when you are seeing many patients. They can help ensure you do not miss anything during your appointments, and you’ll find many of the discussions you have will be the same with a lot of patients, so having quick notes will save you from typing out the same discussion for multiple patients. However, you need to be very careful with how you use these. If you were to be investigated for whatever reason, blank or unfilled areas in your notes would not look very good, and if you have not edited notes to make them specific to each patient’s risks, this could mean some parts of your conversation with the patient may not be there to defend you.
Poor records = poor defence
Something I remember being told when I started working has always stuck with me – Poor records = poor defence. No records = no defence. If you have not written in your clinical notes something you have said, it is essentially assumed the conversation never happened. If you find yourself in the court of law with litigation issues, the only thing there will be to defend you is your clinical notes, or lack thereof, if you are not doing them well.
Further learning
I would really recommend doing some more research and CPD on consent and record-keeping. For good practice guidance, go to the CGDent guidance ‘Clinical Examination and Record-Keeping’ and I would also recommend the indemnity websites where they discuss cases and there is a lot to be learnt from them.
Authors’ bio
“I Graduated from the University of Manchester in 2023, completed my FD Training in the Greater Manchester North Scheme and am now an Associate Dentist in Greater Manchester. I’m also a NextGen Ambassador for the College of General Dentistry. My clinical interests include Oral Surgery and Prosthodontics. I am currently undertaking a Masters in Prosthodontics at UCLAN and have interests in Implants and also dental education. Outside of work, I enjoy running and 5-a-side football.”
Dr Choudhury Rahman

“I graduated from the University of Manchester in 2005 and am currently an Educational Supervisor in Greater Manchester North Scheme, as well as an expert witness. I spend most of my time carrying out general dentistry, alongside placing implants and running two NHS dental practices. Outside work I enjoy spending time with my two boys and I am also an avid Manchester United fan”
Dr Francisco Casserley

References
CGDent guidance – Clinical Examination and Record-Keeping. Available at: https://cgdent.uk/clinical-examination-and-record-keeping/
GDC (2013). General Dental Council – Focus On Standards. [online] gdc-uk.org. Available at: https://standards.gdc-uk.org/.
Theddu.com. (2025). Oro-antral communication after extraction. [online] Available at: https://ddujournal.theddu.com/issue-archive/autumn-winter-2024/oro-antral-communication-after-extraction [Accessed 20 Nov. 2025].
MDU (2024). Montgomery and informed consent – The MDU. [online] Themdu.com. Available at: https://www.themdu.com/guidance-and-advice/guides/montgomery-and-informed-consent.