The College of General Dentistry, GC and The Tom Bereznicki Charitable Educational Foundation would like to congratulate the successful candidates in the 2026 CGDent and GC Award for Foundation Trainees, and thank everyone who entered.
This year, all 14 winning entrants are dentists, who between them studied at eight different dental schools, and who are now completing their Dental Foundation Training or Dental Vocational Training through eight different deaneries across the UK.
| Candidate name | Undergraduate qualification | Educational Supervisor(s) | Deanery |
|---|---|---|---|
| Dr Abdurahman Abdi | BDS Cardiff University 2025 | Dr Sian Blackshaw | Wales |
| Dr Sahand Abolfathi | BDS University of Glasgow 2025 | Dr Bushra Bashir | Scotland |
| Dr Mariam Ahmed | BDS Newcastle University 2025 | Dr Rosie Johnston, Dr Heather Coventry | North East and Cumbria |
| Dr Xiaoyu Foo | BDS University of Dundee 2025 | Dr Iain Bufton | Scotland |
| Dr Esha Gupta | BDS University of Plymouth 2025 | Dr Saleem Mulla | Midlands |
| Dr Joshua Hurley | BDS King’s College London 2025 | Dr Niloy Karia | London and Kent, Surrey and Sussex |
| Dr Anushka Kapour | BDS University of Plymouth 2025 | Dr Deepa Shah, Dr Neil Shah | London and Kent, Surrey and Sussex |
| Dr Daniel Lekhi | BDS University of Birmingham 2025 | Dr Brenda Macmillan, Dr Rebecca Hamilton | Thames Valley and Wessex |
| Dr Lance Lesterpearson | BDS University of Plymouth 2024 | Dr Mohammed Faisal | London and Kent, Surrey and Sussex |
| Dr Aqil Matin | BDS University of Manchester 2025 | Dr Emily McConnell | North West |
| Dr Imane Nagi | BDS University of Birmingham 2025 | Dr Bharat Modhwadia | North West |
| Dr Priyanka Shah | BDS University of Dundee 2025 | Dr Nava Darzi, Dr Hardeep Matharu | East of England |
| Dr Safa Shareef | BDS University of Manchester 2025 | Dr Jemma Hook | North West |
| Dr Heba Turki | BDS Newcastle University 2025 | Dr Neesha Chopra | North East and Cumbria |
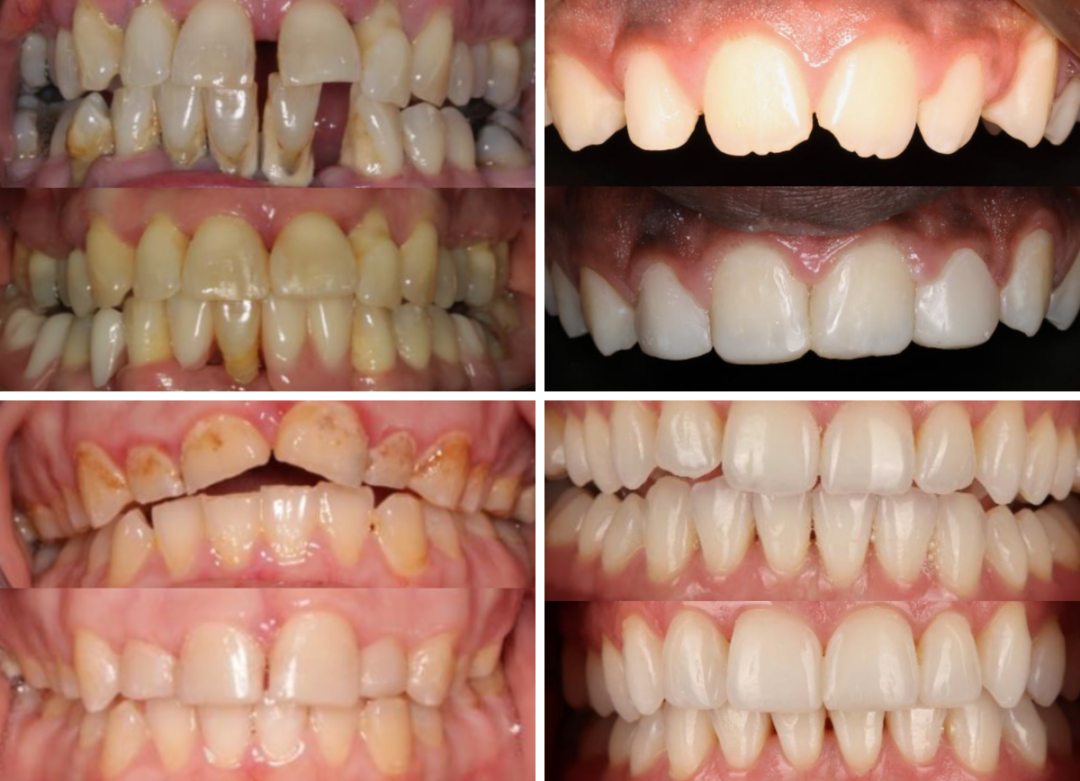
To enter, each participant submitted a restorative case which included at least one anterior tooth restored with composite. Cases entered involved a range of restorative treatments including those for midline diastema, dental trauma, tooth wear and peg shaped laterals. View all successful cases here.
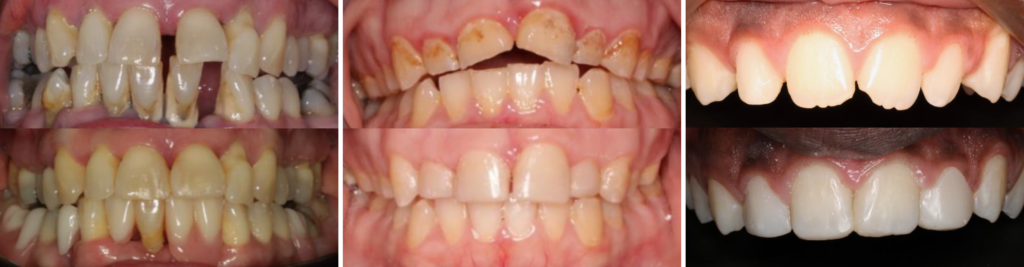
A selection of successful cases which illustrate a range of different types of cases entered in the award. Cases submitted by (L-R) Esha Gupta, Xiaoyu Foo, and Lance Lesterpearson
The award, was open to dentists and dental therapists who graduated in 2025 in the UK and Ireland or who were undergoing Dental Foundation Training, Dental Vocational Training or Joint Dental Foundation Core Training. Entries were received from practitioners from both eligible dental constituencies around the country.
The assessment panel, which comprised Trustees of The Tom Bereznicki Charitable Educational Foundation and senior members of the College, scored each case based on a set of assessment criteria which allocated points to overall improvement in the patient’s oral health (including periodontal health), the standard of aesthetic treatment, the complexity of the case and the quality of the entrant’s reflection.

The successful candidates are each awarded a funded place on a two-day composite layering course which is taking place on 23-24 July at GC’s European Education Campus in Leuven, Belgium. The prize includes international travel and hotel costs and is worth around £1,400 per place.
Shreya Sharma (pictured above left), a winner of last year’s award, described how simply entering the award provided a valuable learning opportunity, “It was a thoroughly rewarding experience, regardless of the outcome I learned a lot about composites by taking part and preparing my case.” Another 2025 winner, Cara Marcuccilli, said, “I’ve learned so much about layering techniques for composite, the different materials we were given the opportunity to use, as well as clinical indications for each technique we practised.”
To register your interest in next year’s award and receive notifications as soon as the competition opens in September, visit our award page.